Health
Diagnosed with adult onset type 1 diabetes: Now what?
By Julie Davis Canter Aug 15, 2022 • 7 min
Hearing you have type 1 diabetes, or T1D, can be both shocking and overwhelming. You’re likely to have a lot of questions. How did this happen? How did I never know until now? What do I do next? Well, you’re not alone in this. Many patients with type 1 diabetes are diagnosed as adults.
How do I suddenly have type 1 diabetes as an adult?
That question might be on a continuous loop in your mind, especially since T1D used to be thought of as a childhood disease. T1D is an autoimmune disease, meaning your immune system misfires and attacks your own body. In this case, it goes after the cells in your pancreas that make insulin. Insulin helps move glucose from the food you eat out of your bloodstream and into your cells. When you don’t produce enough insulin for that transfer, your blood sugar level can spike. It may be a slow process, taking years before symptoms appear.
What causes your immune system to go rogue isn’t well understood. One possibility is that certain genes you were born with suddenly get triggered by something in your environment.
Rest assured that lifestyle choices didn’t cause your T1D, but the choices you make going forward will help you successfully manage this complex condition.
Take control of T1D
Type 1 diabetes management has lots of moving parts, so there’s bound to be a learning curve when you first get started. One of the first steps in living a healthy life with type 1 diabetes is learning how to properly monitor your blood sugar levels, which will help you know when to take your insulin and how much insulin to take.
Blood sugar basics
Blood sugar control will boost energy and improve sleep, mood and concentration. It also helps avoid future health threats like heart disease, kidney disease, eye problems and nerve damage. It can be tricky because levels can fluctuate from the foods you eat as well as the activities you do, exercise included.
You want your numbers just right. For most individuals with type 1 diabetes, this is between 80–130mg/dL before eating and under 180mg/dL two hours afterward. Too high and you risk hyperglycemia with symptoms that could include confusion, headache, extreme thirst, frequent urination, fatigue, irritability and blurry vision. Too low and you risk hypoglycemia, with symptoms that may include confusion and headache, dizziness and lightheadedness, irritability, trouble concentrating, sweating and shaking, a fast heartbeat and, in extreme situations, difficulty speaking and seizures.
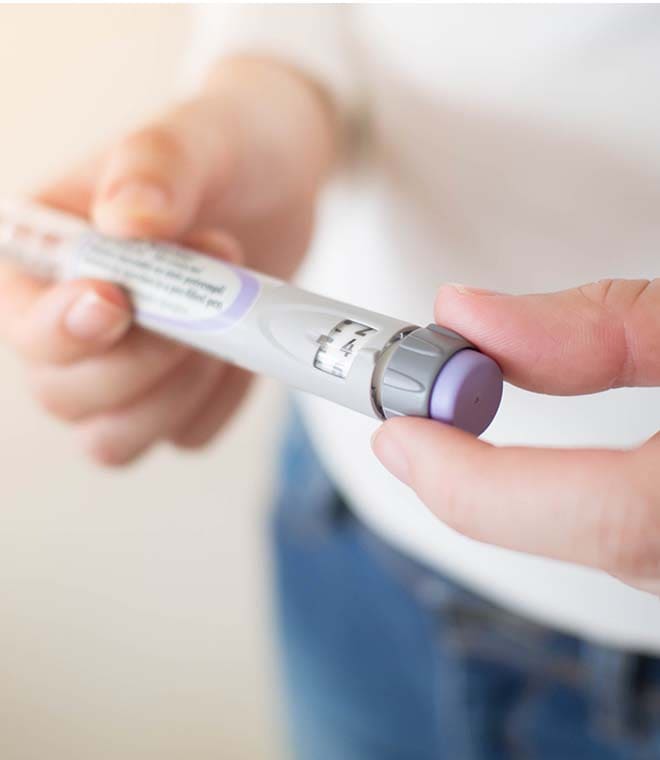
Understanding insulin
Most people need two types:
- Basal insulin, taken once or twice a day, helps keep blood sugar at a consistent level apart from mealtimes
- Prandial insulin, taken before meals, helps stabilize blood sugar after eating
Insulin is described by how quickly and how long it works, with terms like rapid-acting, short-acting or long-acting. Your care team will develop a plan to help you know what you need and when.
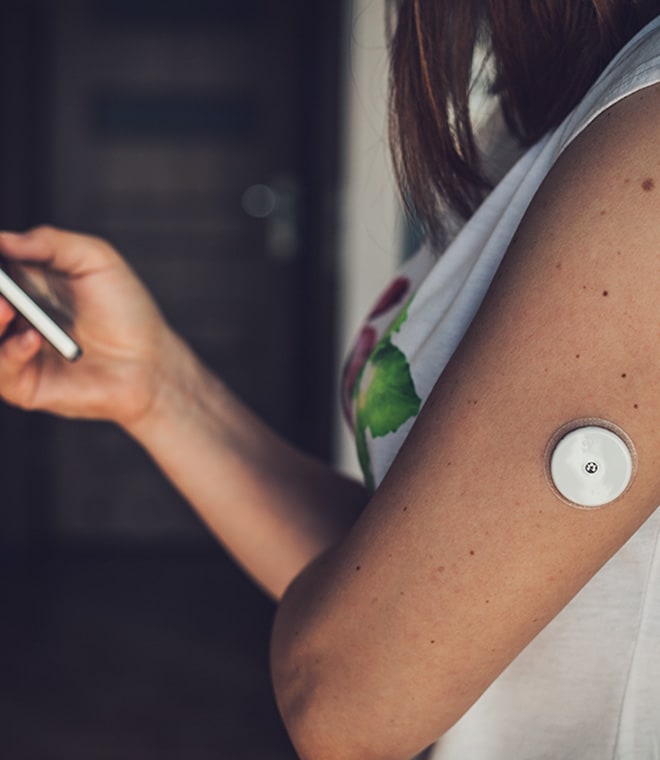
Tapping into high-tech solutions
It used to be that people with type 1 diabetes had to constantly prick their fingers to measure blood sugar with a handheld blood glucose meter and give themselves injections. Today, wearable devices can do most of the work. A continuous glucose monitor (CGM) checks blood sugar around the clock. An insulin pump gives a steady flow of insulin throughout the day and extra doses at mealtimes to help with your rises in blood sugar from the food you eat. You can also give yourself a dose at the press of a button if needed. Most advanced are closed-loop systems, with a CGM, an insulin pump and specialized software that communicate with each other. Also known as automated insulin dosing (AID) systems or artificial pancreas systems, some can be linked with your smartphone.
An AID system can improve two important markers:
- Your A1C number—the blood test result that shows how well you’re controlling blood sugar over a three-month period
- Your TIR (time in range)—how long your blood sugar stays in your target range on any given day
Create a care network
Managing T1D is easier when you have lots of support.
Start with your healthcare team:
- Primary care doctor for routine needs
- Endocrinologist for specialized diabetes treatment
- Other specialists, like a podiatrist (foot doctor) and ophthalmologist (eye doctor)
- Registered dietitian nutritionist
- Certified Diabetes Care & Education Specialist (CDCES)
- Pharmacist
Learn from T1D experts:
Working hand in hand with a certified diabetes educator will enable you to:
- Streamline daily care
- Choose foods for better blood sugar balance
- Exercise safely
- Master blood sugar testing and insulin use
- Spot high/low blood sugar warning signs
- Catch problems early to avoid complications
Also, a diabetes self-management education and support (DSMES) program can quickly get you up to speed. You’ll learn how to overcome care hurdles and emotional ups and downs and protect your overall health. Ask your doctor for a referral or search for a specialist.
Published August 2022.
Sources:
- https://diabetesjournals.org/care/article/40/3/291/36910/Basal-Glucose-Can-Be-Controlled-but-the-Prandial
- https://www.jdrf.org/t1d-resources/about/
- https://www.cdc.gov/diabetes/basics/what-is-type-1-diabetes.html
- https://www.diabetes.org/blog/type-1-diabetes-basics
- https://www.cdc.gov/diabetes/basics/diabetes-type-1-diagnosis.html
- https://www.jdrf.org/t1d-resources/about/facts/
- https://diabetesjournals.org/care/article/44/11/2449/138477/Adult-Onset-Type-1-Diabetes-Current-Understanding
- https://www.mayoclinic.org/diseases-conditions/type-1-diabetes/diagnosis-treatment/drc-20353017
- https://diabetesjournals.org/care/article/40/3/291/36910/Basal-Glucose-Can-Be-Controlled-but-the-Prandial
- https://www.cdc.gov/diabetes/basics/type-1-types-of-insulin.html
- https://www.cdc.gov/diabetes/basics/type-1-4-ways-to-take-insulin.html
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8119627/
- https://www.cdc.gov/diabetes/managing/managing-blood-sugar/a1c.html
- https://www.cdc.gov/diabetes/managing/education.html