Health
Dry skin: Causes, symptoms and treatments
By Anna H. Chacon, MD, Fellow of the American Academy of Dermatology Feb 07, 2025 • 8 min
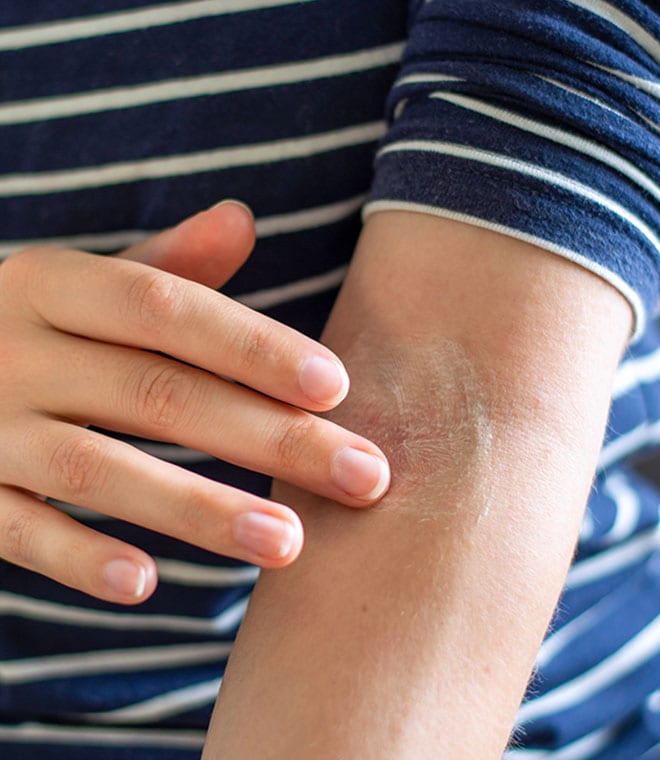
Dry skin, or xerosis, is a common dermatological problem that can occur for short periods throughout the year, or it can persist for longer. There are many causes of dry skin, and fortunately, there are effective ways to help restore and relieve dry skin.
What causes dry skin?
Dry skin occurs when the level of natural oil or sebum isn’t adequate to keep the tissue properly hydrated. Skin may become deprived of moisture for a variety of reasons, including:
Age — Your body naturally produces less sebum as you age. After the age of 40, sebum levels drop significantly, leaving you more likely to develop dry skin, and the risk of xerosis continues to increase the older you get. Hormonal changes related to menopause also contribute to age-related skin dryness in women.
Work and daily activities —Things that you do during the day may cause dry skin or worsen symptoms. Exposure to water and harsh chemicals can strip moisture and protective layers from the skin. As a result, people who wash their hands frequently for work, such as nurses, are more prone to dry skin. Housekeepers, construction workers, hairdressers, florists and cooks may also be more likely to develop dryness.
Even if you don’t work in one of these occupations, you may develop dry skin from completing household chores like washing dishes or scrubbing floors. Simply washing your hands more frequently during cold and flu season may also lead to dryness.
Weather — Some people develop dry skin only during the winter months. This is because cold air retains less moisture than warm air. Drier climates with low humidity, desert-like or windy conditions can also cause excess moisture to evaporate from the skin. This can also occur due to dry heat from furnaces and fireplaces.
Nutritional deficiencies —Itchy, flaky skin can be a symptom of some nutritional deficiencies. Specifically, low levels of niacin, zinc, iron and vitamin A and vitamin D are associated with xerosis. A medical provider can order blood work to check for nutrient levels. If it turns out you are deficient in a key vitamin or mineral, they may recommend that you take a supplement.
Medications — Some prescription drugs increase moisture loss from the skin tissue and raise the risk of dryness. Diuretics, which are often taken for high blood pressure, and cholesterol-lowering statin drugs are two common medications that can cause excessively dry skin as a side effect. Check with your healthcare provider if you begin experiencing dry skin while taking a medication.
Smoking — Harmful substances in cigarette smoke can accelerate the aging process. If this occurs, moisture levels may drop more rapidly as you age.
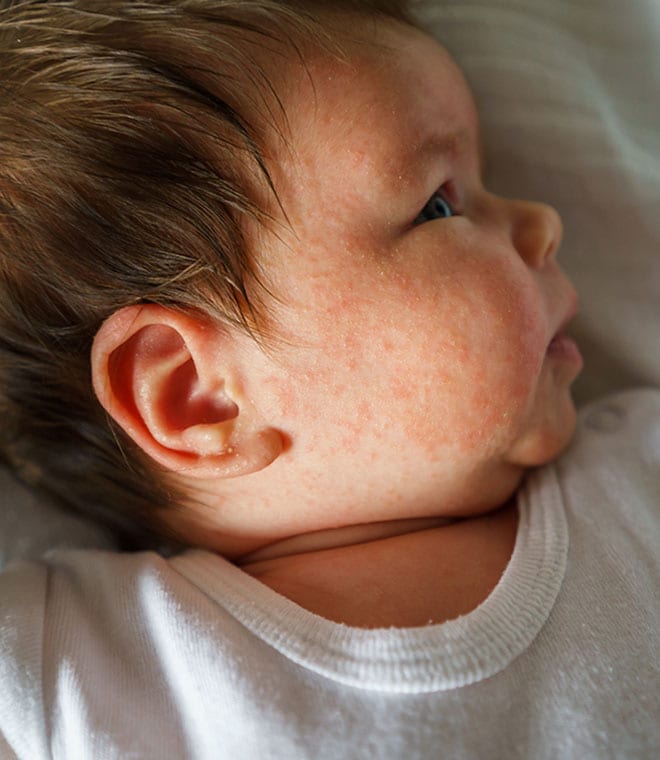
Skin conditions — Many dermatological conditions cause dry skin. Examples include:
- Eczema: An inflammatory skin condition, eczema often causes dry skin patches
- Ichthyosis: A chronic condition marked by scaly skin and excessive dryness
- Perioral dermatitis: Red rash that develops around the mouth
- Psoriasis: An immune system-related disorder, psoriasis causes patches of thickened, flaky and scaly skin to develop
- Seborrheic dermatitis: An inflammatory skin condition that primarily affects the scalp
In some cases, dry skin can actually worsen chronic dermatological conditions. The condition increases the risk of xerosis, and when skin becomes dry, symptoms may grow more severe. As a result, using a moisturizer for dry skin is often a part of a treatment plan for eczema and other conditions.
Medical conditions — Having certain medical conditions can put you at an increased risk of dry skin. Xerosis is a common symptom of both thyroid disease and diabetes. Kidney disease can also cause dryness, especially if you undergo dialysis as a part of your treatment plan. People who are HIV positive are also more likely to develop dry skin.
What can I do about dry skin?
For mild to moderate dryness caused by age or environment, self-care may be enough to resolve symptoms like flaky or scaly skin. Follow these tips to address dryness at home.
Moisturize — Moisturizers replenish hydration levels in the skin. Applying a cream, ointment or moisturizer after a shower can ease symptoms of dryness. You can use a moisturizer in the morning and evening within a few minutes of bathing, showering or washing your hands. You can also reapply moisturizer whenever your skin feels tight or itchy.
Use a humidifier — Increasing humidity levels in your home can supply your skin with added moisture. One option is to invest in a portable cool mist humidifier that you can move from room to room throughout the day and even take to work.
Alter your beauty routine — Your daily routine can improve or worsen dry skin symptoms. To ease dryness:
- Use mild skin care products: Look for cleansers and moisturizers that are hypoallergenic and fragrance-free to decrease the risk of irritation.
- Shorten your showers or baths: Limiting your skin’s exposure to water to five to 10 minutes can reduce moisture loss. Hot water can increase the stripping effect of bathing, so keep the temperature warm but not steaming.
- Treat your skin gently: When drying off after a shower or bath, pat your skin rather than rub. Use a light touch when applying moisturizer. Avoid scratching or picking at dry skin patches.
- Shave at the appropriate time: Save shaving for the end of your shower or bath. This will allow the skin to become clean and softer, which can reduce the risk of irritation.
Your healthcare provider may give you more personalized tips for caring for dry skin.
Protect your skin — Taking steps to reduce your skin’s exposure to harsh weather, water and chemicals can help dry skin heal and reduce the risk of its return. Wear protective gloves when working with harsh substances and water. On cold, windy days, cover as much of your skin as possible.
If you continue to experience dry skin despite self-care efforts, talk to your healthcare provider. They can determine the exact cause of your dry skin and recommend the best treatments for your needs.
You should also let your medical provider know any time that discomfort or rashes from dry skin interfere with your daily activities. They may be able to prescribe anti-itch creams to alleviate symptoms while you follow the treatment plan to address dryness.
Your provider can also help you manage chronic skin conditions that cause dryness, such as eczema. While there may not be a cure for many chronic skin conditions, it is possible to reduce the frequency of flare-ups through self-care, over-the-counter products and prescription medications.
Updated by Julie McDaniel, MSN, RN, CRNI, February 2025.
Sources:
- https://www.aad.org/public/everyday-care/skin-care-basics/dry/dermatologists-tips-relieve-dry-skin
- https://www.aad.org/public/diseases/a-z/dry-skin-treatment
- https://www.aad.org/public/diseases/a-z/dry-skin-causes
- https://www.aad.org/public/diseases/a-z/dry-skin-symptoms
- https://www.merckmanuals.com/professional/dermatologic-disorders/cornification-disorders/xeroderma
- https://www.aad.org/public/everyday-care/skin-care-basics/dry/coronavirus-handwashing
- https://www.aad.org/public/diseases/eczema/types/atopic-dermatitis/symptoms
- https://www.niams.nih.gov/health-topics/ichthyosis
- https://www.aocd.org/page/PerioralDermatitis
- https://www.aad.org/public/diseases/psoriasis/what/symptoms
- https://pubmed.ncbi.nlm.nih.gov/38206142/
- https://www.aad.org/public/diseases/eczema/insider/eczema-summertime
- https://www.aad.org/public/everyday-care/skin-care-basics/hair/how-to-shave
- https://www.ncbi.nlm.nih.gov/books/NBK565884/
- https://www.merckmanuals.com/home/skin-disorders/biology-of-the-skin/effects-of-aging-on-the-skin
- https://www.aad.org/news/cold-weather-and-your-skin